
How Dense Are You?
There’s a movement afoot in America. From Maine to Florida, Texas, Oregon, and many states in between, the ‘Are You Dense?’ nationwide campaign led by the breast cancer advocacy movement is making efforts to enact laws that ensure women receive proper education regarding the significance of breast density, and its association with an increased risk of breast cancer. Breast density varies considerably among women, and can also change over the lifespan as a woman ages. For this reason, physicians should inform women undergoing mammograms of their personal level of breast density.
What is breast density and why is it important?
Breast density refers to the relative proportion of the three main contents of the breast: 1) milk-producing glandular tissue and ducts, 2) stroma—the internal scaffolding of the breast that holds everything in place, and 3) fat tissue which serves as a filler to keep the breast soft and pliable. Breasts that have a relatively high proportion of fat tissue are considered “fatty” or “non-dense”, and breasts that have more glandular tissue and stroma are considered “dense”.
Breast density tends to be higher in premenopausal women and in women taking hormone replacement therapy. As women age, the glandular and stromal components of the breast tend to disappear and the fat component tends to predominate. However, some young women have fatty breasts and some elderly women have dense breasts. Breast density patterns also tend to run in families, so women are likely to notice breast densities similar to their mother or sister.
Efforts to increase public awareness of breast density are also motivated by its association with an increased risk of breast cancer. In fact, women with dense breasts are four times more likely to develop breast cancer than women with fatty, less dense breasts. In addition, breast tissue density influences the ability of both physical examination and screening imaging tools to detect the presence of breast cancer.
How is breast density measured?
Breast density is divided into 4 levels based upon the amount of glandular tissue and stroma compared to the amount of fatty tissue contained within the breast (See Image).
- Level 1 density breast tissue is mainly composed of fatty tissue and contains less than 25% glandular tissue and stroma
- Level 2 breast density contains between 25-50% of glandular tissue and stroma.
- Level 3 breast density contains 51-75% glandular tissue and stroma.
- Level 4 breast density is the most dense breast tissue, and is composed of more than 75% glandular tissue and stroma.
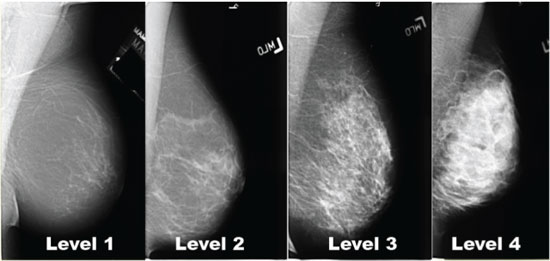
Breast density Levels 1 and 2 are considered “non-dense” due to the high proportion of fatty tissue. The high proportion of fat in Levels 1 and 2 density breasts makes breast cancer detection easier because fat appears gray on a mammogram whereas cancer appears white. Therefore, it’s easy to detect a white cancer against a gray background. On the other hand, the high proportion of glandular tissue and stroma in Level 3 and 4 density breasts makes breast cancer detection more difficult because glandular tissue, stroma, and cancers all appear white on a mammogram. Consequently, it’s harder to detect a white cancer against a white background. High breast density also causes the breast to feel firmer and lumpy, adding to the difficulty of detecting a cancer on physical examination. While digital mammograms are currently still considered to be the single best tool for breast cancer screening, women with dense breasts need to consider the use of other breast imaging studies to aid in the early detection of breast cancer.
You have a right to know
The effort to improve breast cancer detection and prevention led California legislators to pass a Breast Density Bill which requires mammography providers, beginning April 1, 2013, to notify women if they have Level 3 or Level 4 breast density. Women must also be notified that high breast density may increase their risk of breast cancer. Furthermore, the law will require women with Level 3 or 4 density to be informed of other available screening options to improve breast cancer detection. These options include, but are not limited to, contrast-enhanced breast MRI, whole breast screening ultrasound, and tomosynthesis.
Contrast-enhanced MRI uses an intravenous dye and a magnet (not radiation) to reveal patterns of blood flow within the breasts that might be indicative of the presence of a growing cancerous mass. Screening ultrasound uses sound waves (not radiation) through a hand-held or automated ultrasound unit to detect differences in the texture of the breast that might reveal the presence of a cancer. Tomosynthesis uses X-rays and 3-D imaging (rather than 2-D imaging that is normally used in digital mammograms) to improve breast cancer detection. Each screening tool has its advantages and disadvantages. The major disadvantage of using MRI and screening ultrasound is their inability to detect cancer-associated calcifications as well as digital mammograms. For this reason, annual digital mammograms remain highly recommended for early detection of breast cancer. With regard to supplemental imaging, I personally prefer using contrast-enhanced breast MRI because it is highly sensitive and its lack of radiation.
Empowerment with a catch…and a remedy
The California Breast Density Law goes a long way towards empowering women to make informed decisions about their breast health. Unfortunately, the potential benefit of this law is limited by the fact that the Breast Density Law does not require health plans to pay for any supplemental imaging beyond that of mammography. This essentially means that women with Level 3 or 4 density will be required to pay out-of-pocket for supplemental breast screening studies. Fortunately, many breast cancer screening facilities, such as the Los Angeles Center for Women’s Health, have established programs that can significantly reduce the out-of-pocket cost of supplemental imaging for women undergoing screening mammography at their imaging center. To find out more about the breast density screening program at that Los Angeles Center for Women’s Health, please call 213-742-6418.
Now that you know more about breast density, please join me for the next blog for a discussion about hereditary breast cancer and breast cancer gene testing.
You Might Also Enjoy...


Managing Breast Health During a Pandemic

De-escalating Breast Cancer Treatment: Mission Forward


